Dr. James C Johnston and Neurologist Mehila Zebenigus, MD serve as Directors of this NGO, and along with medical malpractice attorney Thomas P. Sartwelle, BA, LLB, and medical ethicist Professor Berna Arda, MD, PhD, have published extensively on the subject of electronic fetal monitoring (EFM) and cerebral palsy, with peer reviewed articles appearing in the Journal of Child Neurology; British Medical Journal; Neurologic Clinics; Maternal Fetal and Neonatal Medicine; Clinical Ethics; Medical Law International; and a number of other publications.
They have lectured on the topic at medical conferences throughout North and South America, Europe, Asia, the Middle East, and Africa, at diverse locations including Addis Ababa, Baku, Coimbra, Los Angeles, Philadelphia, Sao Paulo, Tel Aviv, and Tokyo. Additionally, Global NeuroCare® holds Special Consultative Status with the United Nations ECOSOC, and Drs. Johnston and Zebenigus have provided expert analysis on EFM at several UN meetings over years, including the 2021 High Level Political Forum.
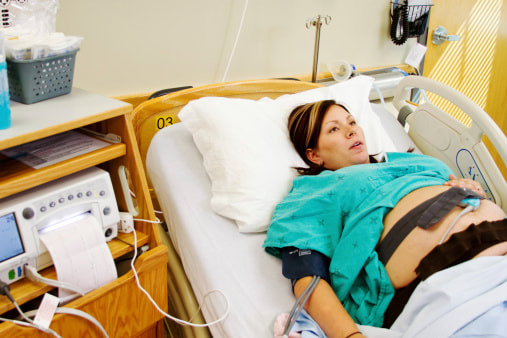
In recent publications, the use of EFM was noted to be a significant contributor to the rising rate of childbirth complications in the US. The rate of C-Sections rose from 6 percent in the 1970s, when EFM was introduced, to 32 percent today, significantly higher in many other countries, which puts increasing pressure on the healthcare system and endangers the lives of both mothers and children.
EFM is ineffective in detecting actual complications during normal pregnancy, and it does not predict or prevent cerebral palsy or any other neurological malady. The false positive rate exceeds 99% leading to many unnecessary C-sections with all of the attendant complications of that procedure, including potential long term consequences for the child.
The continued use of EFM represents an abysmal ethical failure that should be addressed through informed consent and changing the standard of care. If a physician is going to use EFM, then the expectant mother should be told the truth – EFM does not prevent or predict cerebral palsy or any other neurological condition. And an authoritative statement from an International Task Force would allow defendants to bring Daubert junk science challenges against the EFM ‘experts’ who continue testifying that EFM predicts and prevents cerebral palsy. This would be the beginning of the end of EFM litigation.






 RSS Feed
RSS Feed
